Why the USA’s Best Mental Health Billing Services Company Matters More Than Ever in 2026
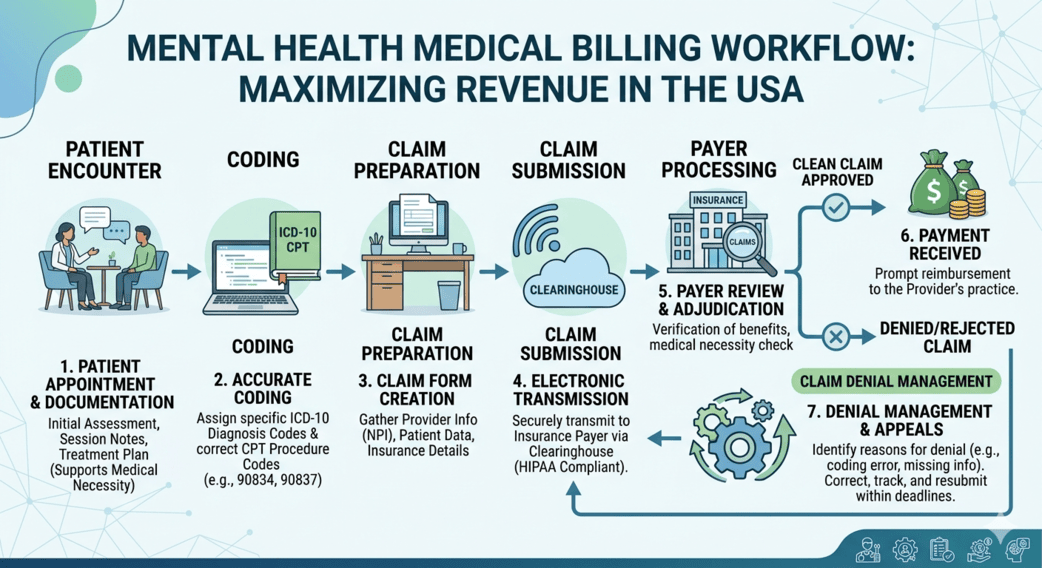
The mental healthcare industry in the USA is evolving rapidly. From private therapy practices and psychiatric clinics to telehealth counseling platforms, providers are handling more patients, more insurance complexities, and stricter compliance requirements than ever before. While the demand for behavioral healthcare continues to rise, reimbursement challenges are becoming equally difficult to manage.
That’s exactly why many providers are searching for the best mental health billing services company to support their practice growth without sacrificing patient care.
Mental health billing is not like standard medical billing. It involves specialized coding, prior authorization requirements, payer-specific behavioral health policies, documentation scrutiny, and complex reimbursement rules. Even a small error can lead to denied claims, delayed payments, or compliance risks.
In this article, we’ll explore what makes a reliable mental health billing partner, why outsourcing has become a strategic move for providers across the USA, and how specialized billing teams help improve revenue performance for behavioral healthcare organizations.
The Growing Complexity of Mental Health Insurance Billing
Behavioral healthcare billing has changed dramatically over the last few years. Insurance carriers now require more detailed documentation, stricter coding accuracy, and faster claim submission timelines.
Providers offering therapy, psychiatry, addiction treatment, counseling, or telepsychiatry services often face challenges such as:
- Frequent claim denials
- Underpaid reimbursements
- Delayed insurance approvals
- Prior authorization complications
- Coding errors for psychotherapy sessions
- Telehealth billing confusion
- Coordination of benefits issues
Because of these challenges, many practices now rely on professional mental health insurance billing services to manage claims efficiently while reducing administrative stress.
A dedicated billing team understands behavioral health payer policies and helps practices avoid common reimbursement mistakes that can quietly drain revenue over time.
Why Specialized Mental Health Billing Matters
General billing companies may understand standard healthcare claims, but behavioral health billing requires deeper expertise.
A qualified mental health billing specialist knows how to handle:
CPT and ICD-10 Behavioral Health Coding
Mental health claims often involve psychotherapy codes, psychiatric diagnostic evaluations, medication management visits, and telehealth modifiers. Incorrect coding can trigger automatic denials.
Time-Based Documentation Requirements
Behavioral health services are highly documentation-sensitive. Session duration, treatment plans, and progress notes must align correctly with billed services.
Telehealth Billing Rules
Virtual counseling and psychiatric care remain heavily utilized across the USA. Each payer has different telehealth reimbursement requirements, making accurate billing critical.
Insurance Verification
Behavioral health benefits vary significantly between policies. A specialized team verifies coverage before appointments to reduce patient billing issues later.
This is why providers increasingly seek a trusted mental health billing services agency instead of relying solely on in-house staff.
Signs You Need to Outsource Mental Health Billing Services
Many providers wait too long before addressing revenue cycle inefficiencies. However, certain warning signs indicate it may be time to outsource mental health billing services.
Claims Are Frequently Denied
If denied claims are becoming routine, your billing workflow may have coding or submission gaps.
Staff Are Overwhelmed
Front-office teams often struggle balancing patient communication with insurance follow-ups.
Payments Are Delayed
Slow reimbursements can impact payroll, operations, and long-term growth.
Revenue Is Unpredictable
Inconsistent collections usually point toward unresolved claim issues or poor denial management.
Providers Spend Too Much Time on Billing
Therapists and psychiatrists should focus on patient care—not chasing insurance companies.
Partnering with a professional mental health billing provider allows practices to regain operational stability while improving financial performance.
Benefits of Outsourced Mental Health Billing
Outsourcing billing has become a practical solution for solo practitioners, group practices, rehabilitation centers, and psychiatric organizations.
A reliable outsourced mental health billing model can provide several advantages.
Improved Claim Accuracy
Experienced billing professionals reduce coding mistakes and improve first-pass claim acceptance rates.
Faster Reimbursements
Claims are submitted promptly and tracked consistently, leading to quicker payments.
Reduced Administrative Burden
Office staff can focus more on patient scheduling and communication instead of handling insurance disputes.
Better Compliance
Behavioral healthcare regulations continue to evolve. Outsourcing helps practices stay updated with payer requirements and HIPAA standards.
Scalable Operations
As practices grow, outsourced billing teams can handle increasing claim volumes without disrupting workflows.
This is one reason why providers continue searching for the top outsource mental health billing company that understands both financial operations and behavioral healthcare compliance.
What Makes the Best Mental Health Billing Agency?
Not every billing company is equipped to handle mental health claims efficiently. Choosing the right partner requires careful evaluation.
Here are the qualities that define the best mental health billing agency in today’s healthcare environment.
Industry-Specific Expertise
Behavioral health billing requires specialized experience. The company should understand psychotherapy coding, psychiatric evaluations, substance abuse treatment billing, and telehealth regulations.
Strong Denial Management Process
The best agencies actively monitor denied claims, identify recurring patterns, and implement corrective strategies to prevent future revenue loss.
Transparent Reporting
Providers should receive regular financial reports that clearly outline collections, denials, reimbursements, and outstanding claims.
Credentialing Support
Insurance enrollment delays can impact revenue significantly. Companies offering credentialing services help providers enroll with payers efficiently and maintain active participation status.
Technology Integration
Modern billing workflows depend on seamless EHR and practice management integration. Efficient software systems reduce manual entry errors and improve claim tracking.
Personalized Support
Every behavioral health practice operates differently. A quality mental health billing consultant takes time to understand workflow challenges and create customized solutions.
Common Billing Challenges for Mental Health Providers
Even highly experienced providers encounter billing problems that affect revenue consistency.
Authorization Delays
Certain therapy and psychiatric services require prior authorization before reimbursement approval.
Incorrect Modifiers
Telehealth and behavioral health modifiers vary among insurance carriers.
Missed Filing Deadlines
Late claim submissions can result in permanent revenue loss.
Coordination of Benefits Errors
Patients with multiple insurance plans create additional billing complexities.
Incomplete Documentation
Payers often request additional records to justify behavioral health services.
A professional mental health medical billing solution helps providers proactively manage these challenges instead of reacting after claims are denied.
Why Small Therapy Practices Are Outsourcing Billing
Smaller mental health practices often struggle the most with administrative responsibilities. Hiring, training, and retaining experienced billing staff can become expensive and time-consuming.
As a result, many therapists and counselors now use specialized billing services for mental health therapists to reduce operational pressure.
Outsourcing offers several practical advantages for smaller practices:
- Lower staffing costs
- Access to experienced billing experts
- Reduced compliance risks
- Improved reimbursement consistency
- Less administrative burnout
For therapists trying to balance patient care with business management, outsourcing creates valuable breathing room.
The Role of Mental Health Billing and Coding Companies
A skilled mental health billing and coding company does far more than submit insurance claims.
Their responsibilities often include:
- Insurance eligibility verification
- Accurate coding review
- Charge entry
- Claim submission
- Payment posting
- Denial management
- Appeals processing
- Accounts receivable follow-up
- Revenue analytics
This comprehensive support improves financial visibility while helping providers maintain healthy cash flow.
How Revenue Cycle Management Impacts Behavioral Health Practices
Billing success is closely tied to the overall revenue cycle.
Strong revenue cycle management services help mental health providers improve every financial stage of the patient journey—from scheduling and eligibility verification to final reimbursement collection.
Effective revenue cycle strategies help practices:
- Reduce denied claims
- Improve reimbursement speed
- Increase collection rates
- Strengthen financial forecasting
- Improve patient billing transparency
Behavioral healthcare organizations that invest in professional revenue cycle management often experience more stable long-term growth.
Why Accurate Medical Coding Matters in Mental Health Billing
Behavioral health coding errors are one of the leading causes of claim denials.
Professional medical coding services ensure accurate use of CPT codes, ICD-10 diagnoses, modifiers, and payer-specific billing requirements.
In mental healthcare, coding accuracy directly affects:
- Insurance reimbursement rates
- Compliance protection
- Audit readiness
- Revenue consistency
- Documentation alignment
An experienced coding team helps providers avoid costly mistakes that may otherwise go unnoticed for months.
Choosing the Best Outsource Mental Health Billing and Coding Company
Before selecting a billing partner, providers should evaluate more than pricing alone.
Important considerations include:
Behavioral Health Experience
Choose a company with direct experience handling psychiatric and therapy billing.
Communication Standards
Reliable support and transparent updates are essential for long-term partnerships.
Reporting Capabilities
Detailed financial insights help providers understand practice performance.
Scalability
The billing company should support future practice growth without workflow disruption.
Compliance Knowledge
HIPAA regulations and payer requirements continue evolving. Your billing partner must stay updated consistently.
The best outsource mental health billing and coding company acts as an operational extension of the practice rather than simply processing claims.
The Future of Mental Health Medical Billing Services
Behavioral healthcare demand across the USA continues to rise. At the same time, insurance carriers are tightening billing oversight and reimbursement requirements.
This means providers will increasingly depend on specialized mental health medical billing services outsourcing partners to remain financially healthy and operationally efficient.
Emerging industry trends include:
- AI-assisted claim review
- Automated eligibility verification
- Predictive denial analytics
- Expanded telehealth billing support
- Real-time revenue reporting
- Integrated behavioral health compliance monitoring
Practices that modernize their billing operations now will be better positioned for long-term success.
Supporting Practice Growth Through Smarter Billing
Financial stability allows mental health providers to focus on what matters most—patient care.
Partnering with a reliable professional mental health billing company helps reduce administrative chaos, improve collections, and streamline insurance workflows.
Many providers are now combining specialized medical billing services, medical billing and coding services, and credentialing services into one integrated operational strategy to improve efficiency across their organization.
By aligning billing, coding, payer enrollment, and compliance management together, practices can create stronger financial foundations while reducing unnecessary stress on internal teams.
Why Providers Are Turning to 247 Medical Billing Services
Across the USA, healthcare organizations are increasingly seeking billing partners that understand the unique challenges of behavioral healthcare reimbursement.
Companies like 247 Medical Billing Services support providers through specialized solutions that include:
- Mental health insurance billing
- Behavioral health coding support
- Revenue cycle management services
- Credentialing services
- Accounts receivable management
- Medical coding services
- End-to-end medical billing and coding services
Rather than functioning as a generic billing vendor, experienced partners help providers create more predictable financial workflows while maintaining compliance standards.
For therapy practices, psychiatric groups, and behavioral health organizations navigating increasingly complex insurance systems, specialized billing expertise has become more important than ever.
FAQs
What are mental health billing services?
Mental health billing services manage insurance claims, coding, payment posting, denial management, and reimbursement processes specifically for behavioral healthcare providers.
Why should therapists outsource mental health billing?
Outsourcing reduces administrative workload, improves claim accuracy, speeds reimbursements, and allows therapists to focus more on patient care.
What does a mental health billing specialist do?
A mental health billing specialist handles behavioral health coding, insurance verification, claim submissions, denial resolution, and payer communication.
How do mental health billing companies improve revenue?
They reduce coding errors, improve clean claim rates, manage denied claims effectively, and optimize the overall revenue cycle process.
What should providers look for in a mental health billing agency?
Providers should evaluate industry experience, compliance expertise, reporting transparency, denial management capabilities, and customer support quality.
Are medical coding services important for mental health practices?
Yes. Accurate coding directly impacts reimbursement accuracy, compliance protection, and claim approval rates for behavioral health providers.
- Courses
- Career & Jobs
- Student Life & Growth
- Technology & Skills
- Health
- أخرى
- Shopping
- Sports
- Wellness


